are also blocked. That clarifies that the body would be exposed to hypoxemia.
It may lead to obtrusive trouble within the anterior and posterior parts of the thorax, depending on the disease's degree and cause. On the other hand, a few individuals may realize the nearness of atelectasis, most regularly considered a chest disease, coming about from a preexisting issue, indeed, even though they are something else sound.
The term “atelectasis” is named after the Greek words “atelēs,” which implies “inadequate,” and the word “ekstasis, ” which is additionally from the same dialect and means “extension.” This contention is invalid because it implies the tightening influences of a portion of the lung. Hence, it isn't able and planning to grow completely.
Restorative science respects atelectasis as an event rather than a malady, but it is found in certain cases particularly. It may be a fundamental condition. It can be intense, persistent, constrained, or asymptomatic, and the sign shifts among individuals. Analyzing this sickness requires considering its causes, sorts, and long-term well-being impacts.
Such atelectasis is often perceived as something minor, not so frequently present in the hospital setting. The most common is postoperative atelectasis, which is found mostly after thoracic or abdominal operations. Given how the body normally functions under anesthesia, normal breathing is reduced, and the lung tissue fills out; thus, atelectasis exists due to this case.
The studies performed to this end have indicated that a significant number of individuals postoperatively also have some level of atelectasis with or without any drug therapy. Some of them may even disappear by themselves.
The illness that comes like a kick starts among those who have already developed chronic conditions like chronic obstructive pulmonary disease (COPD) or asthma.
The kids and OPDers very often have (for them, it is usually more often), and there are many longer cases with both of those groups. It is no longer the same for others only. Inactivity is also a cause of the disorder. Kids and elders have narrow airways, and less lung elasticity is one of the reasons they are likely to have the occurrence of atelectasis. Henceforth, they produce shallow and infrequent breaths and have difficulty in breathing.
The hazard of atelectasis is specifically relative to the disease's seriousness, degree, and real cause. The illness can suddenly disappear in a few gentle cases without causing genuine harm. In any case, when an expansive parcel of the lung is included in the process, it can cause breathing issues. In this way, the lungs cannot supply the body with the proper sum of oxygen. An unremitting condition can result in changeless harm to the lung tissue, leading to lessened lung work over time.
In cases of such illnesses as contaminations, tumors, and inward breath of remote bodies, the requirement for critical restorative mediation may come to avoid the disintegration of well-being, which is inescapable.
The chance of complication is exceptionally high in newborn children or patients with preexisting respiratory disarranges since they may not have sufficient breathing savings to compensate for the oxygen trade impedance legitimately.
There are different types of atelectasis, determined based on the cause and nature of lung collapse. A complete and exact classification of types facilitates the proper selection of the best treatment and the better management of the disease.
The famous type is obstructive atelectasis, which occurs due to mucus plugs, tumors, or foreign bodies that hinder breathing. That damages the alveoli, and the air cannot fill the spaces, causing them to collapse. It is the most common category of atelectasis.
There are two different types of atelectasis: compressive and obstructive. The last is caused by tissue entrapment, while the first is caused by pressure around the lung by an adjacent body organ. It may occur even in the presence of air in the pleural cavity due to lung volume reduction. However, all these issues usually co-occur; for instance, chest injuries normally accompany them.
Surfactant deficiency is a major cause of adhesive atelectasis in infants and adult patients with severe lung diseases such as acute respiratory distress syndrome. Type 2 cells are the main producers of surfactants. Still, they may be inhibited by, for example, poor nutrition, minor damage, or low blood sugar levels. It may particularly occur in premature babies and people who have developed ARDS. The alveoli do not work properly. When there is not enough surfactant, they tend to collapse.
Cicatricial Atelectasis, on the other hand, is a type of illness that occurs when scarring of lung tissues emerges as a result of some scary respiratory illnesses, such as tuberculosis and pulmonary fibrosis. The accumulation of fibrous tissue leads to lung malfunctioning, which cannot stretch.
One possible reason for atelectasis is the accumulation of blood in my lungs. The condition is caused by several different factors that attack the lungs differently. The commonest reason in bedridden patients is the lack of postoperative mobility. Pain and the aftereffects of anesthesia may lead to the depletion of the airway due to poor ventilation after surgery, which causes secretions to build up, resulting in partial lung collapse.
Airway obstruction is another common cause. Mucous plugs, foreign body aspirations, or tumors present air blockage, so insufficient oxygen reaches the alveoli. It is especially common in kids who, by accident, swallow or aspirate easily inhaled substances or people whose mucus production is increased by certain diseases, such as cystic fibrosis.

The atelectasis signs and symptoms differ about the degree of lung insufficiency and the cause (of the condition). There may be no apparent symptoms in mild cases, and the disease is most likely discovered incidentally on other imaging examinations, which are taken for different reasons.
If any symptoms occur, shortness of breath may be the first, which might vary from not strong to very strong. Many times, shallow and fast breathing is the main presentation if the body tries to cope with decreased lung function. In contrast, chest pain may occur on the side that experienced trauma, and in some cases, it is not serious.
Fewer symptoms include coughing, which could be either dry or productive, and cyanosis, a bluish discoloration of the skin and mucous membranes indicating low oxygen levels in the blood. Furthermore, fatigue and general weakness accompany early-stage oxygen deprivation of the body's cellular respiration.
Among the multiple complexities left unchecked, atelectasis might force pneumonia to be one of the most common. When the trapped secretions in the lung lobe do not circulate, it may be jeopardized by some infection. Breathing imposes extra problems, and the recuperation period is prolonged.
Persistent collapse of the lung due to atelectasis may cause permanent lung damage and subsequently decreased lung function. The most likely outcome is bronchiectasis, the infection by the localized cold in the airways. This condition is characterized by dilation and mucus production, obstructing airflow and resulting in frequent infection. Hypoxemia, the condition where the blood is low on oxygen, is another possible infection, especially when atelectasis is present in many cases or is severe. The heart may have to work harder, so there is a strain on the body and organs that may be systemic.
A lung pro, as a rule, takes an exhaustive restorative history and physical exam to analyze atelectasis. A specialist may tune in to the lungs with a stethoscope, listen to the “missing” or “diminished” breath sounds displayed, and recognize the influenced portion. Besides, they may note that bluntness to percussion could be a sign of lung collapse or liquid collection.
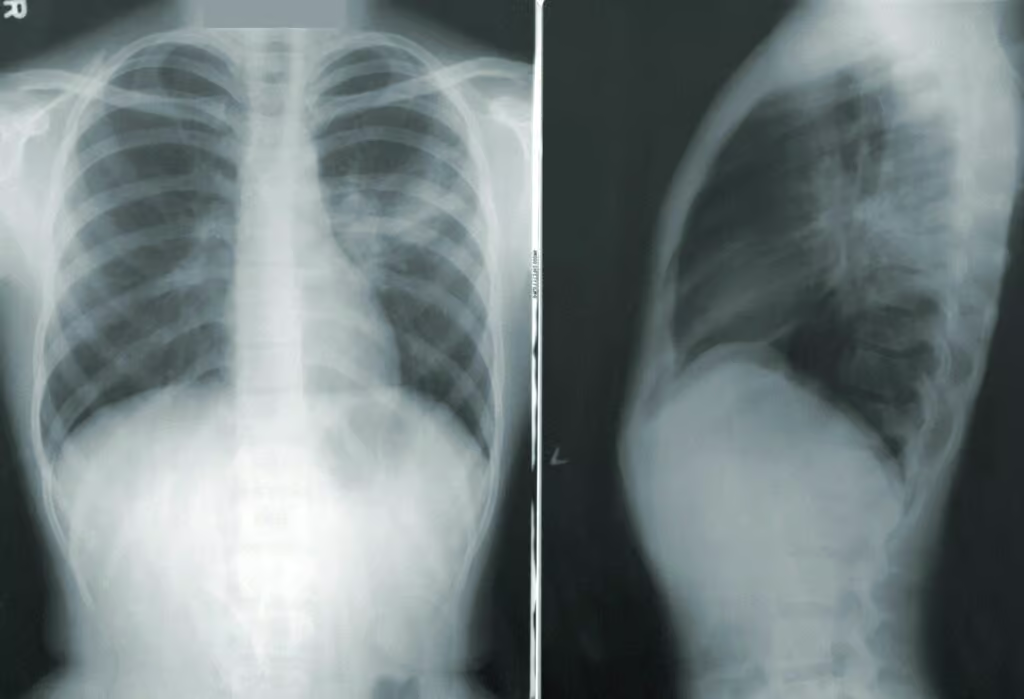
Chest X-rays are, as a rule, the primary imaging tests to be performed. They can show the locale of the lung collapse that would seem darker due to air if they are not showing there, demonstrating the collapse. Whereas the X-rays are helpful for specialists, they sometimes miss minor ranges of atelectasis.
CT imaging filters are more detailed and best represent the state of the lungs. CT is additionally great for uncovering things that cause atelectasis, such as a tumor or a blockage. Too, CT imaging is more delicate to small ranges of the lung that have collapsed, something that a conventional X-ray camera cannot do.
Ultrasound is asked when a healthcare supplier must check someone's condition. It is especially inquired for when the issue is thought to be a pleural emanation, which can lead to compressive atelectasis. This non-invasive and successful method is utilized for imaging and diagnosing in part-filled pleural ranges.
Bronchoscopy is another way of diagnosing atelectasis. It includes employing a lean, adaptable tube with a light and a minor camera to see into the lungs. This procedure permits physicians to require tissue tests, expel objects like bodily fluid plugs, or perform bronchoscopic lavage for foreign body evacuation. In this case, bronchoscopy is the foremost predominant alternative.
Another test that a specialist may inquire about is aspiratory work tests, which are utilized to determine the degree of lung disability. These tests compute the lung volume and airflow and degree of the gas trade to obtain essential data around the gravity of atelectasis and its impact on the complete respirational framework.
The cure of atelectasis mainly relies on the underlying etiology, the extent of lung collapse, and the patient's overall health. No particular treatment is necessary for minor cases since the condition frequently disappears. However, in the case of more critical and persistent medical problems, various measures can be utilized to bring the lungs back to normal and prevent complications.
Blockages caused by bronchus entail bronchoscopy intervention. In this case, a physician may fish out the inflammations, including mucus, tumors, or foreign bodies. Additionally, in cases of pleural effusion or pneumothorax in which the interlobar collapse of the lung is the cause, drainage of the pleural fluid or air space might be required. That can be done through invasive procedures like thoracentesis or chest tube insertion.
Therapeutic agents may also be useful in this direction. Fluticasone increases the airway diameter, mainly in persons with mainstream breathing disorders, such as asthma and chronic obstructive pulmonary disease (COPD). The infections that cause atelectasis, such as pneumonia, need antibiotic therapy.
For patients with long-lasting or recurring atelectasis, an operation might be the better choice. This is especially true if the lung abnormalities and persistent tumors are accounted for. Even though it is an unusual occurrence, a lung resection may be performed to remove non-functioning and damaged parts of the lungs.
Oxygen therapy and supplemental care are the most common methods of providing sufficient oxygen levels, while other kinds of therapy are also given. In general, if the patient's condition is very bad or can't breathe as needed, this machine can assist in breathing until the lungs are well.
Indeed, in spite of the fact that a few cases of atelectasis may vanish without therapeutic intercession, a few signs and indications require prompt restorative help. In a sudden extreme scene, a individual may confront trouble breathing, chest torment, or an unexpected drop within the oxygen level, which would point out genuine atelectasis or indeed a related condition such as pneumonia or respiratory failure.
Patients around to experience surgery must be exceptionally cautious and falter. Short breaths, which cannot be clarified, by the way, and, lastly, in case the state of the lungs is declining at the time of recuperation, are the signs that patients ought to report to a healthcare supplier.
Stop sharing the symptoms of atelectasis with several illnesses, as it is the principal hindrance a doctor faces when diagnosing. A prime example of this disease is pneumonia. It displays the same signs, i.e., coughing, fever, and shortness of breath, just like atelectasis most of the time. On the other hand, pneumonia is caused by the inflammation of lung tissue, while atelectasis occurs when the lung collapses.
Also, a blood clot in the lung, which is called a pulmonary embolism, can be misdiagnosed with asphyxia because it can instantly produce chest pain and breathing difficulty. Antithesis, which is atelectasis with a character of locality, may not only be a risk of previous surgery but also deep vein thrombosis.

Living with atelectasis is a hardship, especially for poor people with constant forms of the disease. Good breathing is the most important thing to improve symptoms and prevent future episodes. Seeing your doctor is the only way to control your lung function and any other problems with atelectasis.
Another way to prevent the disease is to change one's lifestyle. Smoking cessation is one of the most beneficial steps a person can take. It is used to improve lung health and thus cut the risk of complications. Exercise and deep breathing can also help your lungs stay healthy and prevent mucus from sticking.
In addition to treatments prescribed by the doctor, medications like bronchodilators or corticosteroid inhalations can help prevent disease. Ensuring your body is hydrated and having a humidifier at home can help you breathe without problems.
The destiny of an individual with atelectasis depends on a few components. These include the beginning, the significance, and the practical treatment of the malady. In cases of gentle atelectasis, especially those that occur after surgery, the issue may be settled with negligible exterior help, and it incorporates an awesome guess. The typical postoperative case of atelectasis happens after chest surgeries, and it is, as a rule, gone after patients have practiced breathing works and other physical activities.
Diverse choices exist for the ultimate result depending on the review of the infection. If the cause is treated in time, extreme complications aren't predicted. Long-term issues may arise in case unremitting atelectasis is caused by conditions such as pneumonic fibrosis or extreme contaminations. This may result in lung harm and diminished lung capacity, leading to a diminished quality of life.
Children and babies who have the infection are considered to be exceptionally hazardous cases. This is particularly true for those who were born prematurely or have preexisting respiratory maladies. Still, a few of them can feel much way better with the assistance of great medicine. As for each age group, early determination and treatment are basic components of achieving a fruitful result.
Table of Contents