In medical parlance, osteopenia means a reduction in bone mineral density below normal values but up to a certain limit. It is a condition where the level is not as low as in osteoporosis, but it can lead to some health issues. Bone growth is the continuous process of building a skeleton throughout human development. The skeleton we are born with begins forming in the womb and grows until maturity. Any problems in this process can lead to failure to achieve peak bone mass at a young age.
Osteopenia has many causes, though bone density loss mostly happens in adulthood. Bone mass declines slowly after the third decade of life and may continue for many decades into older age. This is a natural process, to be sure, but risk factors can hasten the process and make the symptoms worse. It doesn't matter what the reason is; osteopenia is preventable.
Certain aspects of medical history and medical tests can suggest that bone mineral density may be low. Patients may experience unpleasant symptoms, an important signal for doctors. After it becomes clear that patients have osteopenia, they are taught how to modify their lifestyle. In addition, therapeutic strategies are aimed at preventing the disease from progressing to osteoporosis and subsequent complications.
Bones are mineralized connective tissue forming stiff structural elements. However, like other body parts, our bones are constantly remodeled. Osteoclasts and osteoblasts are bone-lining cells. A disconnect between osteoclast and osteoblast activity leads to osteopenia. Thus, the bone regeneration process is disturbed, and bone mass decreases quantitatively. This process has multiple causes. The osteopenia can be divided into primary and secondary. Learn what can lead to you having osteopenia.
Men and women have their peak bone density at 30 years old. From then onwards, people start to lose bone mass gradually. Bone remodeling is an important physiological process in which old bone is resorbed, and new bone replaces it. With aging, these highly dynamic processes of bone renewal become disrupted.
Bone resorption, where osteoclasts remove old and damaged bone, is a process that takes weeks; thus, bone remodeling is relatively fast. At the same time, osteoblasts are still busy forming new bone, which can take a few months to complete. Osteopenia is the result of these time differences. In addition, those with low bone mass in early adulthood also have a greater risk of developing osteopenia.
Bone mineral density is also, to a degree, bound to genetics. Some individuals have a genetic predisposition to it and a family history of the disorder. Experts say that as much as 80% of an individual's capacity to attain and maintain optimal bone mineralization is determined by genetics. The different factors can also overlap and accelerate the pathological process of bone density loss.
Osteopenia is often diagnosed in women during or after menopause. This may be related to the fact that menopause happens later in life when processes acting on bone density are changed. Despite this, various other additional factors play a role in causing the disease. The body experiences a sudden decline in estrogen due to hormonal changes, which is tied to postmenopausal osteoporosis. This hormone contributes to bone resorption and strengthening. Another important function of estrogen is that it influences calcium metabolism and helps provide enough calcium for the bones.
Keep in mind that osteopenia can form significantly earlier in life. An improper diet low in protein, vitamins, and minerals can reduce bone density. Bone needs calcium, in particular. A deficiency will lead to bone frailty since it is the primary mineral in bones. Vitamin D is another essential nutrient, and it boosts calcium absorption. We receive most of this vitamin by synthesizing it in our skin when exposed to the sunlight. You should also limit or avoid alcohol and smoking, as they are significant risk factors for osteopenia. Thus, a good diet and healthy way of life can prevent you from having bone mineral density below normal values.

The lack or absence of physical activity encourages the decline of bone mineral density. This is why the immobilization of the body due to disability, surgery, or accident will elevate the risk of osteopenia. That is why regular exercise is advised for people at risk, as those who regularly engage in physical activity have greater bone mass and incidence of stronger bones. Still, that must be balanced, and don't go overboard with the exercise as it can also result in losing extra pounds. Individuals with low body mass index seem to have an increased possibility of low bone density.
Some diseases and disorders can also lead to osteopenia. These include malabsorption syndromes, chronic renal failure, thyroid disease, and other issues that cause chronic calcium or vitamin D deficiency. Patients with eating disorders can also be prone to low bone mineral density. In such cases, these underlying disease processes must first be treated to prevent osteopenia.
Medications are also regarded as secondary causes. Specific substances that could be used over time could cause lower bone mineral thickness. Patients should be told about it by their doctor in such cases. These include anti-epileptic drugs and chemotherapeutics. Sometimes, changing to an alternative medication or taking vitamin and mineral supplements might be feasible throughout therapy.
Early symptoms of osteopenia make it somewhat impossible to tell that you might be suffering from it. In patients, the abnormalities are typically detected during routine examinations. As bone density decreases, the problem starts to appear. Patients might then begin to present with multiple symptoms but are not always aware of the reason. However, the sooner osteopenia is detected, the easier it is to treat and prevent dangerous osteoporosis, so it is worth knowing the signs.
Sometimes, the first significant indication of osteopenia comes in the form of back pain. Less dense bones are weaker, and bones tend to be damaged during movement, lifting, and other activities. Some patients experience bone pain, and the most frequent pain symptom is pain in the back. The spine is also a common area for strain. They may even lead to minor vertebral fractures that go undetected. This leads to the vast majority of patients experiencing severe osteoporosis with multiple fractures and chronic back pain before successful treatment is given.
Change of posture is also an important sign of possible osteopenia. As a result of reduced bone density, patients may begin to slouch. Because of slumped posture, they may actually seem shorter. Therefore, a considerable lack of height is additionally another significant indication. In patients with advanced osteopenia, doctors might see kyphosis — a stooped posture where the abdomen protrudes. They can also check for the distance between the ribs and the iliac crest. If the distance between the two is less than 2 cm, it can also be an essential sign of osteopenia during the physical exam.
Those who have osteopenia might be asymptomatic. They see a doctor only if bone fractures occur. An awareness of higher occurrences of some fractures in patients can be the first step toward a correct diagnosis. Such fragile fractures dramatically weaken the patient's quality of life since low-density bones tend to break even after slight injuries. Moreover, they bring a greater mortality hazard, in particular among older individuals. Spine, hip, forearm, or humerus fractures are all examples of severe osteoporotic fractures. Patients then need treatment quickly to save them from the worst.
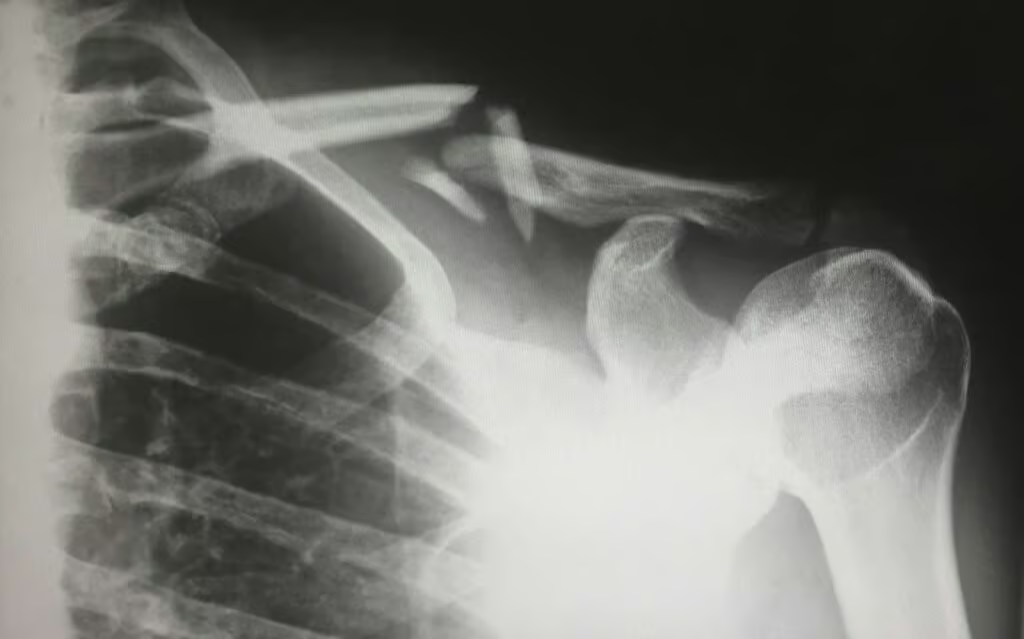
Doctors are required to obtain a comprehensive medical history from patients during the medical examination, taking into account the risk factors for osteopenia (e.g., smoking and chronic alcohol consumption). Also, the family history of the patient having osteoporosis should be incorporated. A patient should be asked for a history of fractures in the past. The physical examination is often normal, except in some cases of advanced disease causing a significant change in posture.
Imaging tests are best in the diagnosis of osteopenia and osteoporosis. Different imaging techniques help to find the fractures. Osteopenia can be detected incidentally on a radiograph showing thin bones or healing fractures. These changes, however, only become apparent when bone mineralization is decreased by at least 20-40%.
Laboratory tests are also used. The biochemical marker that reflects new bone formation due to fast growth or lack of minerals can be used to detect osteopenia in infants. Serum tests can also clear any nutrient deficiencies probably related to low bone density. According to the guidelines, osteopenia is diagnosed when the t-score is between -1 and -2.5, while values below -2.5 are diagnostic for osteoporosis.
Due to the aging population, more people are at risk of bone disorders. Properly preventing and treating osteopenia is certainly critical. Patients with osteopenia may benefit from some basic treatment, including early education on reaching and maintaining a normal bone density level.
Lifestyle changes could be required, but they will pay off in many ways. It is important to educate patients on the appropriate dietary intake or supplementation of calcium and vitamin D. Physicians may encourage patients to quit smoking or alcoholic beverages. They also encourage you to do physical activity with weights and get into your daily workouts.

Patients must also be made aware of ways to prevent harmful falls and, hence, fractured bones. They must ensure that their home environment is safe, for example, by removing obstacles on the ground, such as carpets. Another is correcting vision problems in senior citizens. This is very effective and linked with a lower risk of falls. Physiotherapy actively guides older adults to improve their physical fitness.
Pharmacological treatment is also possible for patients with osteopenia. Over the past few years, the number of proven and safe pharmacological agents for the treatment of osteoporosis has steadily increased. Pharmacotherapeutic agents have an anti-resorptive or anabolic effect, acting on the processes involving osteoclasts and osteocytes. Medication allows patients to decrease the frequency of fractures. Similarly, estrogen therapy can prevent loss of bone mass in menopausal women with osteopenia.
Osteopenia can also be found in children, which is common among adults. Infants born prematurely are especially vulnerable to low bone mineral content and the development of osteopenia. Most bone mineralization, such as the accumulation of calcium and phosphates, occurs during the third trimester of pregnancy. Consequently, babies born before this time have lower reserves of these components. This is why ensuring proper mineral supply at an early age is crucial.
Diagnosing these conditions early on can help prevent fractures in children. Prevention also plays an important role. This means pregnant women must eat foods that can strengthen bones and remember to get some exercise.
In medical parlance, osteopenia means a reduction in bone mineral density below normal values but up to a certain limit. It is a condition where the level is not as low as in osteoporosis, but it can lead to some health issues. Bone growth is the continuous process of building a skeleton throughout human development. The skeleton we are born with begins forming in the womb and grows until maturity. Any problems in this process can lead to failure to achieve peak bone mass at a young age.
Osteopenia has many causes, though bone density loss mostly happens in adulthood. Bone mass declines slowly after the third decade of life and may continue for many decades into older age. This is a natural process, to be sure, but risk factors can hasten the process and make the symptoms worse. It doesn't matter what the reason is; osteopenia is preventable.
Certain aspects of medical history and medical tests can suggest that bone mineral density may be low. Patients may experience unpleasant symptoms, an important signal for doctors. After it becomes clear that patients have osteopenia, they are taught how to modify their lifestyle. In addition, therapeutic strategies are aimed at preventing the disease from progressing to osteoporosis and subsequent complications.
Bones are mineralized connective tissue forming stiff structural elements. However, like other body parts, our bones are constantly remodeled.
Osteoclasts and
osteoblasts are bone-lining cells. A disconnect between osteoclast and osteoblast activity leads to osteopenia. Thus, the bone regeneration process is disturbed, and bone mass decreases quantitatively. This process has multiple causes. The osteopenia can be divided into primary and secondary. Learn what can lead to you having osteopenia.

Men and women have their peak bone density at
30 years old. From then onwards, people start to lose bone mass gradually. Bone remodeling is an important physiological process in which old bone is resorbed, and new bone replaces it. With aging, these highly dynamic processes of bone renewal become disrupted.
Bone resorption, where osteoclasts remove old and damaged bone, is a process that takes weeks; thus, bone remodeling is relatively fast. At the same time, osteoblasts are still busy forming new bone, which can take a few months to complete. Osteopenia is the result of these time differences. In addition, those with low bone mass in early adulthood also have a greater risk of developing osteopenia.
Bone mineral density is also, to a degree, bound to genetics. Some individuals have a genetic predisposition to it and a family history of the disorder. Experts say that as much as
80% of an individual's capacity to attain and maintain optimal bone mineralization is determined by genetics. The different factors can also overlap and accelerate the pathological process of bone density loss.
Osteopenia is often diagnosed in women during or after menopause. This may be related to the fact that menopause happens later in life when processes acting on bone density are changed. Despite this, various other additional factors play a role in causing the disease. The body experiences a sudden decline in
estrogen due to hormonal changes, which is tied to postmenopausal osteoporosis. This hormone contributes to bone resorption and strengthening. Another important function of estrogen is that it influences calcium metabolism and helps provide enough calcium for the bones.
Keep in mind that osteopenia can form significantly earlier in life. An improper diet low in protein, vitamins, and minerals can reduce bone density. Bone needs
calcium, in particular. A deficiency will lead to bone frailty since it is the primary mineral in bones.
Vitamin D is another essential nutrient, and it boosts calcium absorption. We receive most of this vitamin by synthesizing it in our skin when exposed to the sunlight. You should also limit or avoid alcohol and smoking, as they are significant risk factors for osteopenia. Thus, a good diet and healthy way of life can prevent you from having bone mineral density below normal values.

The lack or absence of physical activity encourages the decline of bone mineral density. This is why the immobilization of the body due to disability, surgery, or accident will elevate the risk of osteopenia. That is why regular exercise is advised for people at risk, as those who regularly engage in physical activity have greater bone mass and incidence of stronger bones. Still, that must be balanced, and don't go overboard with the exercise as it can also result in losing extra pounds. Individuals with low body mass index seem to have an increased possibility of low bone density.
Some diseases and disorders can also lead to osteopenia. These include malabsorption syndromes, chronic renal failure, thyroid disease, and other issues that cause chronic calcium or vitamin D deficiency. Patients with eating disorders can also be prone to low bone mineral density. In such cases, these underlying disease processes must first be treated to prevent osteopenia.
Medications are also regarded as secondary causes. Specific substances that could be used over time could cause lower bone mineral thickness. Patients should be told about it by their doctor in such cases. These include anti-epileptic drugs and chemotherapeutics. Sometimes, changing to an alternative medication or taking vitamin and mineral supplements might be feasible throughout therapy.

Early symptoms of osteopenia make it somewhat impossible to tell that you might be suffering from it. In patients, the abnormalities are typically detected during routine examinations. As bone density decreases, the problem starts to appear. Patients might then begin to present with multiple symptoms but are not always aware of the reason. However, the sooner osteopenia is detected, the easier it is to treat and prevent dangerous osteoporosis, so it is worth knowing the signs.
Sometimes, the first significant indication of osteopenia comes in the form of back pain. Less dense bones are weaker, and bones tend to be damaged during movement, lifting, and other activities. Some patients experience bone pain, and the most frequent pain symptom is pain in the back. The spine is also a common area for strain. They may even lead to minor vertebral fractures that go undetected. This leads to the vast majority of patients experiencing severe osteoporosis with multiple fractures and chronic back pain before successful treatment is given.
Change of posture is also an important sign of possible osteopenia. As a result of reduced bone density, patients may begin to slouch. Because of slumped posture, they may actually seem shorter. Therefore, a considerable lack of height is additionally another significant indication. In patients with advanced osteopenia, doctors might see
kyphosis — a stooped posture where the abdomen protrudes. They can also check for the distance between the ribs and the iliac crest. If the distance between the two is less than 2 cm, it can also be an essential sign of osteopenia during the physical exam.
Those who have osteopenia might be asymptomatic. They see a doctor only if bone fractures occur. An awareness of higher occurrences of some fractures in patients can be the first step toward a correct diagnosis. Such fragile fractures dramatically weaken the patient's quality of life since low-density bones tend to break even after slight injuries. Moreover, they bring a greater mortality hazard, in particular among older individuals. Spine, hip, forearm, or humerus fractures are all examples of severe osteoporotic fractures. Patients then need treatment quickly to save them from the worst.

Doctors are required to obtain a comprehensive medical history from patients during the medical examination, taking into account the risk factors for osteopenia (e.g., smoking and chronic alcohol consumption). Also, the family history of the patient having osteoporosis should be incorporated. A patient should be asked for a history of fractures in the past. The physical examination is often normal, except in some cases of advanced disease causing a significant change in posture.
Imaging tests are best in the diagnosis of osteopenia and osteoporosis. Different imaging techniques help to find the fractures. Osteopenia can be detected incidentally on a radiograph showing thin bones or healing fractures. These changes, however, only become apparent when bone mineralization is decreased by at least 20-40%.
Laboratory tests are also used. The biochemical marker that reflects new bone formation due to fast growth or lack of minerals can be used to detect osteopenia in infants. Serum tests can also clear any nutrient deficiencies probably related to low bone density. According to the guidelines, osteopenia is diagnosed when the t-score is between
-1 and -2.5, while values below -2.5 are diagnostic for osteoporosis.
Due to the aging population, more people are at risk of bone disorders. Properly preventing and treating osteopenia is certainly critical. Patients with osteopenia may benefit from some basic treatment, including early education on reaching and maintaining a normal bone density level.
Lifestyle changes could be required, but they will pay off in many ways. It is important to educate patients on the appropriate dietary intake or supplementation of calcium and vitamin D. Physicians may encourage patients to quit smoking or alcoholic beverages. They also encourage you to do physical activity with weights and get into your daily workouts.

Patients must also be made aware of ways to prevent harmful falls and, hence, fractured bones. They must ensure that their home environment is safe, for example, by removing obstacles on the ground, such as carpets. Another is correcting vision problems in senior citizens. This is very effective and linked with a lower risk of falls. Physiotherapy actively guides older adults to improve their physical fitness.
Pharmacological treatment is also possible for patients with osteopenia. Over the past few years, the number of proven and safe pharmacological agents for the treatment of osteoporosis has steadily increased. Pharmacotherapeutic agents have an anti-resorptive or anabolic effect, acting on the processes involving osteoclasts and osteocytes. Medication allows patients to decrease the frequency of fractures. Similarly, estrogen therapy can prevent loss of bone mass in menopausal women with osteopenia.
Osteopenia can also be found in children, which is common among adults. Infants born
prematurely are especially vulnerable to low bone mineral content and the development of osteopenia. Most bone mineralization, such as the accumulation of calcium and phosphates, occurs during the third trimester of pregnancy. Consequently, babies born before this time have lower reserves of these components. This is why ensuring proper mineral supply at an early age is crucial.
Diagnosing these conditions early on can help prevent fractures in children. Prevention also plays an important role. This means pregnant women must eat foods that can strengthen bones and remember to get some exercise.
Table of Contents